FairChoices Methods
Comprehensive technical documentation of the mathematical models and methodologies used in FairChoices
Summary
FairChoices is a deterministic mathematical model of the population that includes demographic and epidemiological parameters taken from international data sources. The model calculates the potential impact of interventions by changing rates of disability and mortality from various causes as a function of the effectiveness of the interventions (taken from the literature) and changes in population coverage (e.g., scaling up intervention X from 30% coverage in 2025 to 80% coverage in 2050).
Analytical Process
Intervention costs are taken from the literature and adjusted to different country settings. The demographic and epidemiological data identify the population in need of each intervention, which along with the coverage assumptions informs the estimates of aggregate costs.
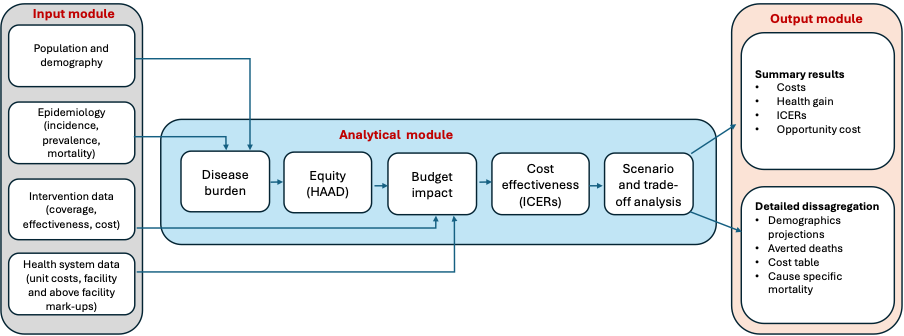
Health Impact Model
Overall Structure of Health Impact Model
Steps that are used in calculation of lifetime health effects:
Defining Age Cohorts
1-year age- and sex-specific mortality and disability rates are adjusted according to increase in target coverage. Future birth cohorts are projected based on baseline mortality and fertility.
Health-adjusted Life Expectancy (HALE) Calculations
For each age cohort, current and future, we calculate sex-specific HALE in the baseline scenario (i.e. no change in coverage) and in the adjusted scenario (i.e. with interventions scaled to target coverage).
Cohort-level HYs Gained
Sex-specific HYs gained are calculated for each cohort in the population by: HYcohort,sex = Ncohort,sex(HALEcohort,sex(target)– HALEcohort,sex(baseline))
Total HYs Gained
Total HYs gained are obtained by summing all the sex- and cohort-specific HYs: HYtotal = Σ(HYcohort,sex)
Statistical Lives Saved (SLS) Calculation
Step 1: Defining Age Cohorts
1-year age- and sex-specific mortality and disability rates are adjusted according to increase in target coverage. Future birth cohorts are projected based on baseline mortality and fertility.
Step 2: Mean Change in Mortality Rates (Mx)
Calculate mean statistical lives saved (SLS) in each current and future age cohort by: Mx = Mx(baseline) – Mx(target)
Step 3: SLS per Age Cohort
Calculate cohort-specific SLS by summing gains for each current and future age cohort: SLScohort = popcohort(baseline) × Mxcohort
Step 4: Total SLS
Total SLS are obtained by summing sex- and cohort-specific SLS: SLStotal = Σ(SLScohort,sex)
Important Note
One artifact with this methodology is that the population is dynamic, meaning births are entering future age cohorts, and interventions improving SLS may create larger future older age cohorts, and this is why you may see negative SLS in older cohorts for some interventions.
Mathematical Details of Health Impact Model
The FairChoices model uses a lifetime perspective on health to capture benefits that last well beyond the implementation period from interventions like HPV vaccination of adolescents, kidney transplant, and obstetric fistula surgery.
Model Foundation
We use a model based on standard lifetable methodology, where input on demography and epidemiology is based on:
- World Population Prospects – for demographic data
- Global Burden of Diseases and Injuries study (GBD) – for epidemiological data
- Medical literature and other data sources – for intervention coverage and effects
Population Cohorts
Assuming a scale-up period of 25 years and that mortality is 100% at age 100, we consider 126 cohorts:
- C0 through C100 – cohorts that are alive today
- C-1 through C-25 – cohorts that will be born during the next 25 years
Key Mathematical Formulations
eadj = ecrude × (covtarget – covbaseline) / (1 – (ecrude × covbaseline))
Mx = Mx,background + Mx,cause
Mx,adjusted = Mx,background + Mx,cause × (1 – eadj)
SLSy = Ny × Σ(Mx – Mx,y)
Total SLS = Σ(SLSy) for y = -25 to 100
HLYs gainedy = HLEadjusted,y – HLEbaseline,y
Health Effect Models
In FairChoices, we use 9 different effectiveness models:
1. High Urgency Effects
Interventions used in critical care situations where timing is important, and may affect mortality and disability. (e.g. treatment of pneumonia or diarrhea)
2. Future Cohort Prevention
Interventions given at one point of time, but effects come later in life of the cohort. (e.g. vaccines)
3. Treatment AND Prevention Effects
Interventions given at one point of time, but effects both accrue to people with a disease and benefits later in life of the cohort. (e.g. treatment of Hepatitis C, Apocillin to treat StrepB tonsillitis and prevent Rheumatic heart disease)
4. Non Curative – Short Term Effects
Chronic care interventions saving lives, may also improve disability, and increasing prevalence (e.g. HIV treatment, antihypertensives)
5. Non Curative – Long Term Effects
Interventions saving lives, may also improve disability, and has effects beyond the interventions period (e.g. orthopedic surgery, kidney transplant, cancer)
6. Non Curative – Disability Only
Chronic care interventions only affecting disability (e.g. treatment of rheumatoid arthritis)
7. Fertility Effect
Interventions affecting fertility. (e.g. family planning)
8. Indirect Effect – Quality
Interventions with indirect effectiveness on other interventions, necessary to achieve optimal quality of affected interventions (e.g Essential Emergency Critical Care)
9. Indirect Effect – Access
Important interventions without direct health effects per se, necessary to detect conditions and to achieve target coverage. (e.g. universal screening, diagnostics)
Detailed Examples
Prevent Acute Condition for Full Cohort Over a Period of More Than 1 Year
Action: Reduce mortality and disability for whole cohort for duration of PRM (PRM>1)
Example: If PRM=15 for BCG vaccine to infants, and the intervention is provided to infants in a birth cohort, then prevalence of TB will be reduced in this whole birth cohort for 15 years. After 15 years, we assume that mortality in the birth cohort reverts back to baseline mortality.
Immediate Treatment of Incident Cases
Action: Reduce mortality and/or disability for all ages treated in the year of treatment (PRM=1)
Examples: Treatment of diarrhea or arthritis
Long-term Treatment of Deadly Chronic Conditions
Action: Reduce mortality for all age-groups for duration of PRM (PRM>1). The effect within cohort is reduced by a certain fraction per year to account for the fact that new cases in years 2 to PRM were not treated the initial year.
Example: If we provide everyone aged 50 in year 1 in need of a kidney transplant with a new kidney, the mortality in that age cohort will be reduced for 15 years (assuming PRM=15).
Demographic Projection Model
The demographic model uses the cohort component projection method (CCPM) based on the primary determinants of population dynamics: fertility, mortality, and migration. The initial population structure is based on the 2022 World Population Prospects by the UN Population Division.
Key Components
Population Structure
1-year age brackets from 0 to 100 years, segmented by sex, based on World Population Prospects 2022
Fertility Calculations
Age-specific fertility rates (ASFR) provided by WPP. Number of births calculated by: B(t) = Σ(ASFRf(a,t) × Pf(a,t)) for a = 15 to 49
Mortality Survivorship
Life table survivor rates S(a,t) give probability of surviving from age a to age a+1: Ps(a+1,t+1) = Ps(a,t) × Ss(a,t)
Migration Adjustment
Net migration Ms(a,t) incorporated for each age and sex: Ps*(a+1,t+1) = Ps(a+1,t+1) + Ms(a,t+1)
Model Foundation
The CCPM provides a comprehensive account of how a population would evolve differently in baseline and adjusted scenarios, depending on the interventions and coverage targets chosen.
Cost Model
Our cost model follows the approach outlined by Watkins and colleagues in DCP3. We searched the literature for estimates of annual unit costs and adjusted them for health system strengthening costs.
Cost Adjustment Formula
ci = (1 + α) × ci,lit × (1 + β)
Component Breakdown
- α (Facility-level indirect costs): 7.4% for outpatient, 27% for inpatient facilities
- β (Above-facility costs): 17% for supply chain, financing, governance
Country Adjustment
ci,y = δ × ci,x × (Sy / Sx) + (1 − δ) × ci,x
Population-level Cost Calculation
Ci,pop = Σ(ci,k × wi,k × pi,k)
Discounting
- Costs: Discounted by 5% annually
- Health outcomes: Not discounted (0%)
- Time horizon: 5 years with progressive discounting
Limitations
Key Limitation: Economies of Scale
A significant limitation is the lack of empirical data concerning economies (and diseconomies) of scope and scale in the context of Non-Communicable Disease (NCD) interventions.
Specific Limitations
- Economies of Scope: Potential for cost savings in interventions with similar delivery characteristics, but empirical validation is challenging
- Economies of Scale: More readily demonstrated in national-level programs for communicable diseases, but very little is known about NCD programs
- Constant Marginal Costs: Our model assumes constant marginal costs concerning coverage, though marginal costs likely differ at very low and high coverage levels
Mitigation Approach
Despite these limitations, our analysis focused on modest (10-20%) increases in coverage from 2023 to 2030, providing a more justifiable basis for assuming constant marginal costs within this range.
References
[1] Watkins et al. Disease Control Priorities, 3rd Edition. World Bank Group, 2017.

